Rationale for Treatment: Indications and Contraindications
The toxic products released by the microorganisms (From A) are destructive to the periapical tissue. This periapical area (B) is surrounded by C and D. The delicate balance favoring Zones A and B will allow the continuous existence of periapical pathosis, although zone D is capable of repairing the area. Thus, elimination of Zone A (the source of the infection) by endodontic therapy will tip the balance to favoring the activity of Zone D, resulting in repair of the periapical tissue and retention of the tooth.
Fish Diagram: in an experimental situation
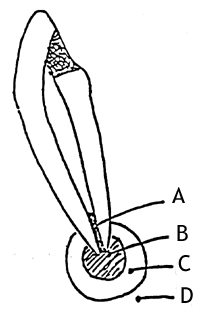 |
Zone A: Area of Infection (PMN and microorganisms) Zone B: Area of Contamination (round cells, toxins and lymphocytes) Zone C: Area of Irritation (histiocytes, osteoclasts, toxins and some normal cells) Zone D: Area of Stimulation (fibroblasts, osteoblasts, and collagen fibers) |
Zone A: Area of Infection (PMN and microorganisms) Zone B: Area of Contamination (round cells, toxins and lymphocytes) Zone C: Area of Irritation (histiocytes, osteoclasts, toxins and some normal cells) Zone D: Area of Stimulation (fibroblasts, osteoblasts, and collagen fibers)
Factors Determining Case Selection:
Assuming a clinician is competent and capable of performing excellent endodontic therapy, the following considerations have to be made when selecting a case for endodontic therapy.
The Patient's:
- Motivation
- Financial ability
- Age
- Physical Disability
- Occupation
- Physical Disorders
Contraindications:
- Inadequate periodontal support: little or no periodontal support with Class III mobility
- Extremely poor condition of the remaining dentition
- Vertical fracture
- Nonrestorable teeth: deep horizontal fracture or deep decay below the alveolar bone level
- Nonstrategic tooth
- Extreme root resorption
- Limited accessibility: e.g. TMJ disorders
- Hypercalcification
- Root perforation
- First trimester pregnancy: give emergency treatment and wait until second trimester to complete root canal therapy
Pathophysiology of Pulp Diseas
 |
-
Intact-Uninflamed Pulp:
Pulps in which the cells appear to be unaltered are classified as "intact-uninflamed"; normal, palisading, tall, columnar, odontoblastic layer, minimal amount of collagen fibers, normal caliber blood vessels and structurally distinct fibroblasts.
Frequently, a dentist encounters an "atrophic pulp". This pulp has shrunken to a fraction of its original volume due to a large amount of reparative dentin formation. No inflammatory signs are observed in this case.
-
Insults:
Any external and internal factors which trigger pathologic processes of the pulp. They may be grouped as follows:
- Physical
- Chemical
1) Phosphoric acid and acrylic monomer
2) Erosion (acids)
- Microbial
1) Caries
-
Acute Pulpitis (Acute Pulpalgia):
A severe toothache is referred to as acute pulpitis. Since acute pulpitis is a clinical condition, the term Acute Pulpalgia is more accurate, because it describes the clinical entity and not the histopathologic diagnosis, as the term "pulpitis" does.
Acute pulpalgia develops mainly from various dental procedures including mechanical pulp exposures. The pain is sharp, throbbing and generally severe. The histopathological picture is a mixture of acute and chronic inflammatory cells. Local destruction and displacement of odontoblasts occur.
Other terms for Acute Pulpalgia: Acute Serous Pulpitis & Acute Suppurative Pulpitis
-
Transitional Stage:
Pulps in which chronic inflammatory cells are detected but are not present in sufficient quantity. Pulps of most teeth with deep carious lesions without any clinical symptoms fall into this category.
The inflammatory response is reversible if the carious lesions are completely excavated and a sedative filling is placed.
-
& 6. Chronic Pulpitis:
- Total Necrosis:
-
Periapical Pathosis (PAP):
PAP is not identical with PAR (Periapical Radiolucency). PAP is characterized by (1) thickening or loss of lamina dura and (2) bone and/or root resorption.
In general, if a long-duration chronic inflammation "leaks out" of the confines of the canal, then the PAP results.
A. Mechanical
1) Trauma (accidental or iatrogenic dental procedures)
2) Pathologic wear (abrasion, etc.)
3) Cracked tooth
4) Barodontalgia
B. Thermal
1) Heat from dental procedures
2) Heat from cement setting
3) Deep filling with no base
4) Polishing
Chronic pulpitis usually develops from untreated deep caries. The pathosis is usually confined to a limited area, the coronal portion of the pulp underlying the region of the involved dentinal tubules, i.e., Chronic Partial Pulpitis. Eventually, the entire pulp becomes involved, i.e., Chronic Total Pulpitis. When a small region of liquefaction, i.e., microabscess, develops within the inflamed pulp, the histological term changes to Partial Liquefaction Necrosis. At this stage, painful symptoms may, but do not necessarily arise. However, if partial liquefaction necrosis develops within total pulpitis, painful symptoms usually follow. In young people, irritation of the chronically inflamed exposed tissue, which has an ample blood supply, leads to the proliferating granulomatous tissue (Chronic Hyperplastic Pulpitis or Pulp Polyps). The same pathosis in old people is called Ulcerative Pulpitis.
Total necrosis represents cells in the pulp which have died as a result of coagulation and/or liquefaction. Coagulation necrosis is described as fixed and opaque protoplasm of the cells with disappearance of the intracellular detail. Liquefaction necrosis is described as replacement of the cells by a dense zone of PMN leukocytes together with the chronic inflammatory cells.
Dry: most likely as a result of trauma
Wet: bacterial infection
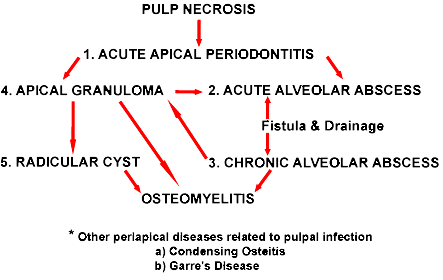
Pathophysiology of Periapical Tissue
 |
-
Acute Apical Periodontitis (AAP):
This acute inflammation usually results from an irritation via the root canal. The causes may be root canal instrumentation or a high filling. The other possible causes are formocreosol irritation of periapical tissue or extrusion of bacteria from the apex during biomechanical procedures. The clinical symptom is pain, especially to percussion, which makes chewing extremely painful. An adjustment of the occlusion is the treatment of choice.
The histopathological picture shows the dilation of blood vessels together with PMN infiltration and an accumulation of exudate. The tooth may be extruded slightly due to the exudate.
X-ray: No significant changes.
-
Acute Alveolar Abscess (AAA):
(Acute Suppurative Apical Periodontitis):The reaction of the periapical tissue to the infection, AAA, is a localized collection of pus in the alveolar bone at the root apex of a tooth following pulpal death. The initial clinical symptoms are slight tenderness, in the later stages, severe throbbing pain with attendant swelling of the overlying soft apical tissue occurs. The pus may break through a fistula, i.e. a fistulous tract.
To diagnose the involved tooth, a gutta percha cone is inserted into the tract and an x-ray is taken. Due to the absorption of toxic products from the abscess, a general systemic reaction may occur, e.g. a slight fever, chills, malaise and headaches. Due to the abscess, the tooth may be extremely mobile. The histopathological picture shows the marked infiltration of PMN, rapid accumulation of exudate and empty spaces where suppuration has occurred.
X-ray: Slight thickening of PDL
-
Chronic Alveolar Abscess (CAA)
(Chronic Suppurative Apical Periodontitis):This is a long-standing low-grade infection of the periapical alveolar bone due to the root canal infection or pulpal necrosis. There are generally no clinical symptoms and a fistulous tract may or may not be present.
The histopathologic picture shows the accumulation of plasma cells and lymphocytes at the periphery, and disintegrating PMN at the center of the abscess, accompanied by vessel dilation in the PDL. Complications may include osteomyelitis, cellulitis and bacteremia.
X-ray: PAR begins to develop
-
Apical Granuloma
(Chronic Apical Periodontitis):This is a localized mass of chronic granulation tissue, not a tumor, formed in response to the pulpal infection. The tooth is either totally asymptomatic, or sensitive to percussion. PAR is always present.
The histopathologic picture shows infiltration of chronic inflammatory cells, apical bone resorption together with the proliferation of fibroblasts and endothelial cells, mobilization of mononuclear phagocytes, accumulation of cholesterol crystals and the presence of epithelium. If the inflammatory reaction persists, stimulating the epithelium, a radicular cyst may develop.
X-ray: Appears identical to the periapical cyst; PDL thickening at the root apex, PAR with well circumscribed lesion, or diffuse PAR and some degree of root resorption.
-
Radicular Cyst:
This true cyst (epithilial lining of the cystic cavity filled with fluid) is the sequela of the periapical granuloma as a result of pulp necrosis with infection.
Granuloma epithelial rests of Malassez degeneration and liquefaction of central epithelial cells due to lack of nutrient cyst
Clinical symptoms: asymptomatic
Histopathology: The epithelial lining of the cavity of the cyst.
Hyaline body (Thrombus)
Lymphocytes & plasma cell infiltration.
X-ray: PAR