Columbia Doctors: Telehealth
Overview
Post-pandemic, ColumbiaDoctors
established an organization-wide goal of increasing telehealth usage, ideally
to achieve 20-25% patient visit volume. With appointment lead times of 30+ days
in several specialties, ColumbiaDoctors worries about
patient leakage to competing hospitals and patient dissatisfaction as these
issues affect not only revenue, but also their reputation when it comes to
providing top-level and timely care.
Objective
Our client representative, both a
practicing physician and a digital health advocate on the leadership board,
tasked us with developing actionable models to increase telehealth adoption
among the >1,800 physicians affiliated with ColumbiaDoctors.
Approach
We conducted primary research by
interviewing current employees of ColumbiaDoctors. We
focused on two specialties, Gynecological Oncology and Vascular Surgery, and
our interviewees spanned different roles within those practices, including
practice managers, mid-level providers (such as nurse practitioners), front
desk secretarial staff, and attending physicians. In our interviews, we sought
to understand the current state of and attitudes towards telehealth, pain
points currently inhibiting greater usage, and opinions on what methods would
or would not work in each practice.
Problem
From our primary research we
surfaced key obstacles preventing further adoption of telehealth at ColumbiaDoctors, from both the patient and provider
perspective. However, to narrow the scope of the project, we decided to focus
on provider pain points as we had direct access to physicians/staff that would
allow us to easily trial and implement proposed changes given the short time period of this project. From the provider perspective,
key barriers are:
●
Lack of perceived benefit of
telehealth by providers
●
Lack of provider capacity on
existing appointment templates
●
Lack of standardized approach
between physicians within a medical practice, but also between practice types
●
Lack of adequate technology for
telehealth
Solution
Through our primary research, we
learned that each specialty has different needs, and on a granular level there
is an extreme amount of variability between the needs of physicians even within
the same specialty. We acknowledge that a one-size-fits-all model would not
work in this scenario. Thus, we built five different models based on the four
key pain points identified through our research:
- Batched
mid-level provider blocks
- Batched
attending blocks
- Attending
office hours
- On-demand
urgent care
- Added
telehealth-only resources
Furthermore, we pressed
practitioners on what variables would make a given model work for their
practice versus another and developed a framework outlining six key practice
parameters and the directional value (low vs mid vs high) of each parameter
best suited to each model (Figure 1):
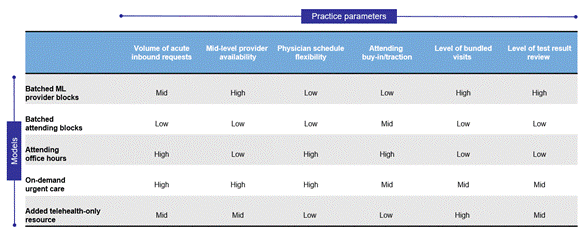
Figure 1. Models and their
characteristics
Our developed models are listed in
the leftmost column, and parameter characteristics are listed in the top row.
To see which model is recommended based on this framework, practitioners can
use the Excel tool we developed (Figure 2) and select a dropdown value of low,
mid, or high for each parameter. An example practice is illustrated in gray
under “Vascular Surgery,” where volume of inbound requests is selected as
“high” while mid-level provider availability is “low”. The tool then calculates
a fit score for each model based on the overlap with the stated practice
parameters, and the model with the highest fit is recommended.
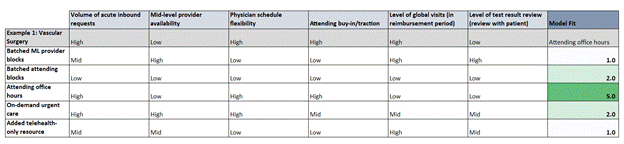
Figure 2. Excel tool developed to
help practitioners choose their best fit model
Conclusion
We developed a process framework
inclusive of a decision making tool that is adaptable
to many different practice types at ColumbiaDoctors. Our proof of concept
endeavor has generated encouraging metric improvements in two different
surgical practice types, as well as an organization-wide initiative to provide
iPads to all practitioners lacking adequate video technology. From the feedback from our pilot studies, we
are learning of the emerging barriers as well as successes from our
recommendations and look forward to keeping in touch with our client to
continue to hear of their progress. Continuing on, we
hope ColumbiaDoctors will continue to use telehealth
as a lever to increase patient access and healthcare equity, and ultimately
look at a follow-up project addressing patient barriers, as those who could
benefit the most from telehealth are often those who most lack the requisite
technology and digital literacy required.