Diabetes Prevention
Lifestyle Modification
In those at high risk for developing diabetes or who have pre-diabetes, insulin secretion may be adequate to maintain fasting blood glucose levels below 126 mg/dL but the process of insulin resistance is already present. High risk individuals need to become aware of interventions to limit the progression to diabetes. In people with impaired glucose tolerance, they should be counseled on the benefits of modest weight loss (5 – 7% loss of body weight) and increasing physical activity. Weight loss and regular exercise can reduce the risk of diabetes by almost 50%.
Drug Therapy
There is increasing evidence that high risk patients may limit progression to type 2 diabetes using glitazones and metformin that target insulin resistance; however cost effectiveness has not yet been fully demonstrated.
For patients with IFG or IGT pre-diabetes, the ADA consensus panel currently recommends lifestyle modification including 5% to 10% weight loss and moderate intensity physical activity approximately 30 min/day.
The panel recommends lifestyle modification and metformin (850 mg twice per day) for individuals with IFG and IGT and any of the following:
- <60 years of age
- BMI ≥35 kg/m²
- family history of diabetes in first-degree relatives
- elevated triglycerides, reduced high density lipoprotein cholesterol
- hypertension
- A1C >6.0%.
If metformin is to be used, both IFG and IGT must be documented. Currently, the panel recommends that only metformin be considered as drug therapy for combined IFG and IGT based on effectiveness, safety, tolerability, and cost.
Follow Up Monitoring
Routine monitoring should be performed with A1C testing semi-annually in individuals with IFG/IGT being treated with metformin. Those who are not receiving drug therapy should be seen annually. These patients should also be assessed and treated for other cardiovascular risk factors (ex. hyperlipidemia, hypertension, tobacco use). Follow up counseling is also important for success of lifestyle modification.
Signs and Symptoms of Undiagnosed Diabetes
Most individuals with undiagnosed diabetes are asymptomatic. Undiagnosed glucose intolerance and persistent hyperglycemia may eventually lead to classic symptoms of increased thirst, polyuria, fatigue, weight loss, and blurry vision. Acanthosis nigricans is a skin change that can occur in those with insulin resistance. Other signs may include obesity, evidence of metabolic syndrome or cardio vascular disease.
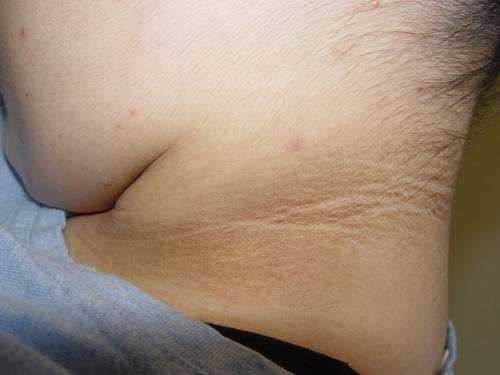
Acanthosis Nigricans from DermAtlas
Diabetes Care
The Initial Evaluation
As per the American Diabetes Association, the goals of a
comprehensive medical evaluation in a patient with a diagnosis of diabetes are:
- to classify the patient
- to detect the presence or absence of diabetes complications
- to assist in formulating management plans
- to provide the basis of ongoing care
Components of the comprehensive diabetes evaluation (ADA Recommendations 2006)
Medical history
- Symptoms, results of laboratory tests, and special examination results related to the diagnosis of diabetes
- Prior A1C records
- Eating patterns, nutritional status, and weight history; growth and development in children and adolescents
- Details of previous treatment programs, including nutrition and diabetes self-management education, attitudes, and health beliefs
- Current treatment of diabetes, including medications, meal plan, and results of glucose monitoring and patients’ use of data
- Exercise history
- Frequency, severity, and cause of acute complications such as ketoacidosis and hypoglycemia
- Prior or current infections, particularly skin, foot, dental, and genitourinary infections
- Symptoms and treatment of chronic eye; kidney; nerve; genitourinary (including sexual), bladder, and gastrointestinal function (including symptoms of celiac disease in type 1 diabetic patients); heart; peripheral vascular; foot; and cerebrovascular complications associated with diabetes
- Other medications that may affect blood glucose levels
- Risk factors for atherosclerosis: smoking, hypertension, obesity, dyslipidemia, and family history
- History and treatment of other conditions, including endocrine and eating disorders
- Assessment for mood disorder
- Family history of diabetes and other endocrine disorders
- Lifestyle, cultural, psychosocial, educational, and economic factors that might influence the management of diabetes
- Tobacco, alcohol, and/or controlled substance use
- Contraception and reproductive and sexual history
Physical examination
- Height and weight measurement (and comparison to norms in children and adolescents)
- Sexual maturation staging (during pubertal period)
- Blood pressure determination, including orthostatic measurements when indicated, and comparison to age-related norms
- Fundoscopic examination
- Oral examination
- Thyroid palpation
- Cardiac examination
- Abdominal examination (e.g., for hepatomegaly)
- Evaluation of pulses by palpation and with auscultation
- Hand/finger examination
- Foot examination
- Skin examination (for acanthosis nigricans and insulin-injection sites)
- Neurological examination
- Signs of diseases that can cause secondary diabetes (e.g., hemochromatosis, pancreatic disease)
Laboratory evaluation
- A1C
- Fasting lipid profile, including total cholesterol, HDL cholesterol, triglycerides, and LDL cholesterol
- Test for microalbuminuria in type 1 diabetic patients who have had diabetes for at least 5 years and in all patients with type 2 diabetes; some advocate beginning screening of pubertal children before 5 years of diabetes
- Serum creatinine in adults (in children if proteinuria is present)
- Thyroid-stimulating hormone in all type 1 diabetic patients; in type 2 if clinically indicated
- Electrocardiogram in adults, if clinically indicated
- Urinalysis for ketones, protein, sediment
Referrals
- Eye exam, if indicated
- Family planning for women of reproductive age
- Medical nutrition therapy as indicated
- Diabetes educator, if not provided by physician or practice staff
- Behavioral specialist, as indicated
- Foot specialist, as indicated
- Other specialties and services as appropriate
Management
A physician-coordinated multi-disciplinary approach is recommended for providing care for patients with diabetes. Multi-disciplinary teams may include a physician, nurse practitioner, physician’s assistant, nurses, nutritionist, pharmacists, mental health specialists and a social worker. The individual with diabetes should assume an active role in their care in collaboration with the team. Care should be tailored for the individual’s needs and involve family and other support systems as allowed by the patient. The patient and the team should understand and agree to the management plan and goals in advance. All plans should recognize the paramount importance of diabetes self management, patient education, and lifestyle modifications.